293 public records – page 1 of 15. — Log in to view all records
- Published Date
- 2011-11-14
- Link to File
- https://www.youtube.com/watch?v=FXjLeFQFPAQ
- Description
- "A video presentation on how to use the 5 Whys to discover the root causes underlying an issue."
- Corporate Author
- 2020 Delivery Academy
- Published Date
- 2011-11-14
- Topics
- Quality Improvement
- Resource Type
- Video Recording
- File Type
- Web page
- Link to File
- https://www.youtube.com/watch?v=FXjLeFQFPAQ
- Originating web page
- http://divisionsbc.ca/provincial/resources/assessment-measurement/root-cause-analysis
- Recording Length
- 4min, 7sec
- Description
- A video presentation on how to use the 5 Whys to discover the root causes underlying an issue.
The 10 Building Blocks of High-Performing Primary Care - Article
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource1120
- Published Date
- 2018-06-19
- Description
- "A supporting article to the presentation made during the Primary Care Awakens - Blue Sky Clinic Model Webinar. It highlights the essential elements of primary care, which are called the 10 building blocks of high-performing primary care."
- Personal Author
- Dr Thomas Bodenheimer, Amireh Ghorob, Rachel Willard-Grace, Dr Kevin Grumbach
- Published Date
- 2018-06-19
- Event
- Primary Care Awakens - Blue Sky Clinic Model Webinar
- Resource Type
- Article
- File Type
- Web page
- Originating web page
- http://www.annfammed.org/content/12/2/166.full
- Publisher
- Annals of Family Medicine
- Citation
- Bodenheimer T, Ghorob A, Willard-Grace R, Grumbach K. The 10 building blocks of high-performing primary care. Ann Fam Med 2014. Online.
- Description
- A supporting article to the presentation made during the Primary Care Awakens - Blue Sky Clinic Model Webinar. It highlights the essential elements of primary care, which are called the 10 building blocks of high-performing primary care.
The 12 Attributes of a Patient Medical Home in BC
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource916
- Published Date
- 2016-09-20
- Description
- "This illustration shows the framing of a patient medical home in BC. It depicts one goal and 12 attributes grouped into three areas. The patient is located in the centre, with the goal being whole-person care."
- Corporate Author
- General Practice Services Committee
- Published Date
- 2016-09-20
- Resource Type
- Info Graphic
- File Type
- Originating web page
- http://www.gpscbc.ca/what-we-do/primary-care-bc/patient-medical-home
- Description
- This illustration shows the framing of a patient medical home in BC. It depicts one goal and 12 attributes grouped into three areas. The patient is located in the centre, with the goal being whole-person care.
Accessing Treatment: What do Providers Experience? - Info Graphic
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource1464
- Published Date
- 2017
- Description
- "A high-level visual illustration of the provider’s perspective into the many ways people can access treatment for substance use."
- Corporate Author
- Ministry of Mental Health and Addictions
- First Nations Health Authority
- General Practice Services Committee
- Ministry of Health
- BC Patient Safety & Quality Council
- Published Date
- 2017
- Topics
- Primary Care
- Community / Patient Navigation
- Community Resources
- Adverse Childhood Experiences
- Children and Youth
- Mental Health and Substance Use
- Resource Type
- Info Graphic
- File Type
- Description
- A high-level visual illustration of the provider’s perspective into the many ways people can access treatment for substance use.
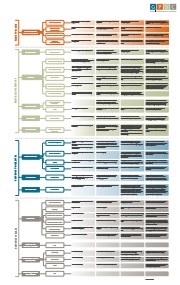
BC PMH Practice Characteristics Matrix Poster
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource1082
- Program
- Practice Support Program
- Published Date
- 2018-04-20
- Description
- "The PMH Practice Characteristics Matrix supports physicians to understand what the 12 attributes of the PMH model mean in concrete terms in the context of their practice, and what a transition towards the PMH could entail for them. As well, it helps GPSC and other health system partners to organize their thinking around the practice-level realities of the PMH model, and the strategic development of provincial supports for physicians to achieve the model. The Matrix—intended to be read from left to right--illustrates both the 12 attributes of the PMH model, as well as their corresponding sub-attributes, several of which are to be achieved cumulatively."
- Program
- Practice Support Program
- Corporate Author
- General Practice Services Committee
- Published Date
- 2018-04-20
- Topics
- Patient Medical Home
- Resource Type
- Poster
- File Type
- Description
- The PMH Practice Characteristics Matrix supports physicians to understand what the 12 attributes of the PMH model mean in concrete terms in the context of their practice, and what a transition towards the PMH could entail for them. As well, it helps GPSC and other health system partners to organize their thinking around the practice-level realities of the PMH model, and the strategic development of provincial supports for physicians to achieve the model. The Matrix—intended to be read from left to right--illustrates both the 12 attributes of the PMH model, as well as their corresponding sub-attributes, several of which are to be achieved cumulatively.
BC PMH Practice Characteristics Matrix with Cover Page
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource1081
- Program
- Practice Support Program
- Published Date
- 04-20-2018
- Description
- "The PMH Practice Characteristics Matrix supports physicians to understand what the 12 attributes of the PMH model mean in concrete terms in the context of their practice, and what a transition towards the PMH could entail for them. As well, it helps GPSC and other health system partners to organize their thinking around the practice-level realities of the PMH model, and the strategic development of provincial supports for physicians to achieve the model. The Matrix—intended to be read from left to right--illustrates both the 12 attributes of the PMH model, as well as their corresponding sub-attributes, several of which are to be achieved cumulatively."
- Program
- Practice Support Program
- Corporate Author
- General Practice Services Committee
- Published Date
- 04-20-2018
- Topics
- Patient Medical Home
- Resource Type
- Report
- File Type
- Description
- The PMH Practice Characteristics Matrix supports physicians to understand what the 12 attributes of the PMH model mean in concrete terms in the context of their practice, and what a transition towards the PMH could entail for them. As well, it helps GPSC and other health system partners to organize their thinking around the practice-level realities of the PMH model, and the strategic development of provincial supports for physicians to achieve the model. The Matrix—intended to be read from left to right--illustrates both the 12 attributes of the PMH model, as well as their corresponding sub-attributes, several of which are to be achieved cumulatively.
The BC Primary Care Research Network: A Vehicle for Innovation and Transformation - Presentation
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource1107
- Health Authority
- Vancouver Coastal
- Division
- Vancouver Division of Family Practice
- Published Date
- 2018-04-17
- Description
- "A presentation from the GPSC Summit 2018 on how divisions, health system partners, health professionals, and patients can get support from BC’s Primary Health Care Research Network to advance their health care innovations."
- Health Authority
- Vancouver Coastal
- Division
- Vancouver Division of Family Practice
- Corporate Author
- Vancouver Division of Family Practice
- University of British Columbia (UBC)
- Fraser Health Authority
- Ministry of Health
- Canadian Primary Care Sentinel Surveillance Network
- Personal Author
- Dr Sabrina Wong Dr Fiona Duncan Shana Ooms Annette Garm
- Published Date
- 2018-04-17
- Event
- GPSC Summit 2018
- Workshop
- The BC Primary Care Research Network: A Vehicle for Innovation and Transformation
- Resource Type
- Presentation
- File Type
- PowerPoint
- Description
- A presentation from the GPSC Summit 2018 on how divisions, health system partners, health professionals, and patients can get support from BC’s Primary Health Care Research Network to advance their health care innovations.
Best Advice Guide on Recovery-Oriented Mental Health and Addiction Care in the Patient’s Medical Home
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource1171
- Published Date
- 2018/10/23
- Description
- "This document provides guidance for offering Mental Health & Addiction services using a recovery-oriented approach in the context of the PMH."
- Corporate Author
- Mental Health Commission of Canada (MHCC)
- College of Family Physicians of Canada
- Published Date
- 2018/10/23
- Resource Type
- Guide
- File Type
- Web page
- Originating web page
- https://patientsmedicalhome.ca/files/uploads/BAG_Mental_Health_ENG_web.pdf
- Description
- This document provides guidance for offering Mental Health & Addiction services using a recovery-oriented approach in the context of the PMH.
Blue Sky Clinic Building - Primary Care Plus - Webinar Presentation
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource1118
- Health Authority
- Island
- Division
- Nanaimo Division of Family Practice
- Published Date
- 2018-06-19
- Link to File
- /media/divresources/PrimaryCareAwakens.pdf
- Description
- "A presentation from the Primary Care Awakens - Blue Sky Clinic Model Webinar on a new model of care designed to inspire engagement of early career family physicians into full service family practice."
- Health Authority
- Island
- Division
- Nanaimo Division of Family Practice
- Personal Author
- Dr Derek Poteryko, Dr Danielle Downe, Dr Shelly Chopra
- Published Date
- 2018-06-19
- Event
- Primary Care Awakens - Blue Sky Clinic Model Webinar
- Resource Type
- Presentation
- File Type
- Link to File
- /media/divresources/PrimaryCareAwakens.pdf
- Description
- A presentation from the Primary Care Awakens - Blue Sky Clinic Model Webinar on a new model of care designed to inspire engagement of early career family physicians into full service family practice.
Boundary Proof of Concept Patient Medical Home/ Primary Care Network: A summary of evaluation findings
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource1179
- Health Authority
- Interior
- Division
- Kootenay Boundary Division of Family Practice
- Published Date
- 2019-01-08
- Link to File
- /media/divresources/BoundaryPoCProvincialSummary.pdf
- Description
- "The document was provided during the GPSC Patient Medical Home Evaluation Webinar. It draws on the GPSC case study of the Boundary PoC in 2018."
- Health Authority
- Interior
- Division
- Kootenay Boundary Division of Family Practice
- Corporate Author
- General Practice Services Committee
- Kootenay Boundary Division of Family Practice
- Published Date
- 2019-01-08
- Event
- GPSC Patient Medical Home Evaluation Webinar
- Resource Type
- Summary
- File Type
- Link to File
- /media/divresources/BoundaryPoCProvincialSummary.pdf
- Description
- The document was provided during the GPSC Patient Medical Home Evaluation Webinar. It draws on the GPSC case study of the Boundary PoC in 2018.
Boundary Proof of Concept Patient Medical Home/Primary Care Networks - Case Study
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource1395
- Health Authority
- Interior
- Division
- Kootenay Boundary Division of Family Practice
- Published Date
- 2019/02
- Link to File
- /media/divresources/BoundaryPoCCaseStudy.pdf
- Description
- "This case study is broken into the following main sections: 1) overview of case study approach, 2) Overview of Boundary PoC design and implementation, 3) Key outcomes achieved to date, 4) Key Boundary PoC successes, 5) Key enablers of success in the Boundary PoC process, 6) Key Boundary PoC challenges; and 7) Conclusions and recommendations."
- Health Authority
- Interior
- Division
- Kootenay Boundary Division of Family Practice
- Corporate Author
- General Practice Services Committee
- Kootenay Boundary Division of Family Practice
- Interior Health Authority
- Published Date
- 2019/02
- Resource Type
- Case Study
- File Type
- Link to File
- /media/divresources/BoundaryPoCCaseStudy.pdf
- Description
- This case study is broken into the following main sections: 1) overview of case study approach, 2) Overview of Boundary PoC design and implementation, 3) Key outcomes achieved to date, 4) Key Boundary PoC successes, 5) Key enablers of success in the Boundary PoC process, 6) Key Boundary PoC challenges; and 7) Conclusions and recommendations.
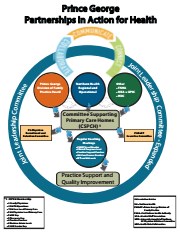
Building a System of Primary Care: Regional Partnership Perspectives - Infographic Handout
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource987
- Health Authority
- Northern
- Division
- Prince George Division of Family Practice
- Published Date
- 2017-06-19
- Description
- "Handout from one of several table discussion during the Building a System of Primary Care: Regional Partnership Perspectives session at the GPSC Spring Summit 2017."
- Health Authority
- Northern
- Division
- Prince George Division of Family Practice
- Corporate Author
- Prince George Division of Family Practice
- Northern Health Authority
- Published Date
- 2017-06-19
- Topics
- Engagement
- Patient Medical Home
- Event
- GPSC Spring Summit 2017
- Workshop
- Building a System of Primary Care: Regional Partnership Perspectives
- Resource Type
- Info Graphic
- Handout
- File Type
- Description
- Handout from one of several table discussion during the Building a System of Primary Care: Regional Partnership Perspectives session at the GPSC Spring Summit 2017.
Building a System of Primary Care: Regional Partnership Perspectives - Roadmap Handout
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource986
- Health Authority
- Interior
- Division
- Central Interior Rural Division of Family Practice
- Central Okanagan Division of Family Practice
- East Kootenay Division of Family Practice
- Kootenay Boundary Division of Family Practice
- South Okanagan Similkameen Division of Family Practice
- Thompson Region Division of Family Practice
- Shuswap North Okanagan
- Published Date
- 2017-06-19
- Description
- "Roadmap handout from one of several table discussion during the Building a System of Primary Care: Regional Partnership Perspectives session at the GPSC Spring Summit 2017."
- Health Authority
- Interior
- Division
- Central Interior Rural Division of Family Practice
- Central Okanagan Division of Family Practice
- East Kootenay Division of Family Practice
- Kootenay Boundary Division of Family Practice
- South Okanagan Similkameen Division of Family Practice
- Thompson Region Division of Family Practice
- Shuswap North Okanagan
- Corporate Author
- Interior Health Authority
- General Practice Services Committee
- Published Date
- 2017-06-19
- Topics
- Engagement
- Patient Medical Home
- Event
- GPSC Spring Summit 2017
- Workshop
- Building a System of Primary Care: Regional Partnership Perspectives
- Resource Type
- Plan
- Handout
- File Type
- Word
- Description
- Roadmap handout from one of several table discussion during the Building a System of Primary Care: Regional Partnership Perspectives session at the GPSC Spring Summit 2017.
Building Blocks for Maternity Care - Presentation
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource1113
- Health Authority
- Fraser
- Interior
- Division
- Burnaby Division of Family Practice
- Kootenay Boundary Division of Family Practice
- White Rock South Surrey Division of Family Practice
- Published Date
- 2018-04-17
- Description
- "A presentation from the GPSC Summit 2018 on the several initiatives that are improving maternity care for providers and patients."
- Health Authority
- Fraser
- Interior
- Division
- Burnaby Division of Family Practice
- Kootenay Boundary Division of Family Practice
- White Rock South Surrey Division of Family Practice
- Corporate Author
- General Practice Services Committee
- Burnaby Division of Family Practice
- Kootenay Boundary Division of Family Practice
- White Rock South Surrey Division of Family Practice
- Personal Author
- Dr Shelley Ross Nancy Falconer Kim Williams Dr Charlene Lui Dr Marvin Lemke Dr Jeanette Boyd Dr Tahmeena Ali Dr Karen Buhler
- Published Date
- 2018-04-17
- Event
- GPSC Summit 2018
- Workshop
- Building Blocks for Maternity Care
- Resource Type
- Presentation
- File Type
- Description
- A presentation from the GPSC Summit 2018 on the several initiatives that are improving maternity care for providers and patients.
Building Collaborative Leadership
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource1598
- Program
- Practice Support Program
- Published Date
- 2018
- Description
- "This tool helps teams to identify characteristics of different collaborative leadership approaches and set areas of focus to help them move towards collaborative leadership."
- Program
- Practice Support Program
- Corporate Author
- General Practice Services Committee
- Published Date
- 2018
- Resource Type
- Tool
- File Type
- Description
- This tool helps teams to identify characteristics of different collaborative leadership approaches and set areas of focus to help them move towards collaborative leadership.
Burnaby DoFP Neighbourhood Networks Case Study - Executive Summary
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource1605
- Division
- Burnaby Division of Family Practice
- Published Date
- 2022-02
- Description
- "This document is the executive summary of the Burnaby DoFP Neighbourhood Networks case study. As part of GPSC commitment to the development of physician networks as a key component of primary care system change, the Burnaby DoFP Neighborhood Network case study explores the development and implementation of three neighborhood networks in Burnaby. The creation of neighborhood networks in Burnaby was prompted by family physicians who recognized the need to bring together family physicians from across local communities to increase their interconnectedness, provide opportunities for local Primary Care Network planning, and enable methods for sharing care with each other with the goal of improving patient access to medical care across Burnaby. Burnaby’s neighborhood networks have supported family physicians to connect socially, learn from each other, identify options for locum coverage and after-hours care, and support referrals to specialist care throughout the networks. Key outcomes: family physicians were able to increase patients’ access to care by referring patients to their family physician peers, expanding their use of locums, working on the development of an Urgent and Primary Care Clinic, and procuring additional healthcare resources for the neighborhood networks. A discussion of the neighborhood network's future goals and next steps is included."
- Division
- Burnaby Division of Family Practice
- Corporate Author
- General Practice Services Committee
- Published Date
- 2022-02
- Resource Type
- Summary
- File Type
- Description
- This document is the executive summary of the Burnaby DoFP Neighbourhood Networks case study. As part of GPSC commitment to the development of physician networks as a key component of primary care system change, the Burnaby DoFP Neighborhood Network case study explores the development and implementation of three neighborhood networks in Burnaby. The creation of neighborhood networks in Burnaby was prompted by family physicians who recognized the need to bring together family physicians from across local communities to increase their interconnectedness, provide opportunities for local Primary Care Network planning, and enable methods for sharing care with each other with the goal of improving patient access to medical care across Burnaby. Burnaby’s neighborhood networks have supported family physicians to connect socially, learn from each other, identify options for locum coverage and after-hours care, and support referrals to specialist care throughout the networks. Key outcomes: family physicians were able to increase patients’ access to care by referring patients to their family physician peers, expanding their use of locums, working on the development of an Urgent and Primary Care Clinic, and procuring additional healthcare resources for the neighborhood networks. A discussion of the neighborhood network's future goals and next steps is included.
Burnaby DoFP Neighbourhood Networks Case Study - Full Report
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource1606
- Division
- Burnaby Division of Family Practice
- Published Date
- 2022-02
- Description
- "This document details the full case study on the Burnaby DoFP Neighborhood Networks. As part of GPSC commitment to the development of physician networks as a key component of primary care system change, the Burnaby DoFP Neighborhood Network case study explores the development and implementation of three neighborhood networks in Burnaby. The creation of neighborhood networks in Burnaby was prompted by family physicians who recognized the need to bring together family physicians from across local communities to increase their interconnectedness, provide opportunities for local Primary Care Network planning, and enable methods for sharing care with each other with the goal of improving patient access to medical care across Burnaby. Burnaby’s neighborhood networks have supported family physicians to connect socially, learn from each other, identify options for locum coverage and after-hours care, and support referrals to specialist care throughout the networks. Key outcomes: family physicians were able to increase patients’ access to care by referring patients to their family physician peers, expanding their use of locums, working on the development of an Urgent and Primary Care Clinic, and procuring additional healthcare resources for the neighborhood networks. A discussion of the neighborhood network's future goals and next steps is included."
- Division
- Burnaby Division of Family Practice
- Corporate Author
- General Practice Services Committee
- Published Date
- 2022-02
- Resource Type
- Case Study
- File Type
- Description
- This document details the full case study on the Burnaby DoFP Neighborhood Networks. As part of GPSC commitment to the development of physician networks as a key component of primary care system change, the Burnaby DoFP Neighborhood Network case study explores the development and implementation of three neighborhood networks in Burnaby. The creation of neighborhood networks in Burnaby was prompted by family physicians who recognized the need to bring together family physicians from across local communities to increase their interconnectedness, provide opportunities for local Primary Care Network planning, and enable methods for sharing care with each other with the goal of improving patient access to medical care across Burnaby. Burnaby’s neighborhood networks have supported family physicians to connect socially, learn from each other, identify options for locum coverage and after-hours care, and support referrals to specialist care throughout the networks. Key outcomes: family physicians were able to increase patients’ access to care by referring patients to their family physician peers, expanding their use of locums, working on the development of an Urgent and Primary Care Clinic, and procuring additional healthcare resources for the neighborhood networks. A discussion of the neighborhood network's future goals and next steps is included.
Capturing the Patient Experience Instruction
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource1371
- Published Date
- 2016
- Link to File
- http://www.hqontario.ca/Portals/0/Documents/qi/qi-capturing-patient-experience-instruction-sheet-en.pdf
- Description
- "This article describes how to capture the patient experience and it is important"
- Corporate Author
- Health Quality Ontario
- Published Date
- 2016
- Topics
- Quality Improvement
- Resource Type
- Article
- File Type
- Link to File
- http://www.hqontario.ca/Portals/0/Documents/qi/qi-capturing-patient-experience-instruction-sheet-en.pdf
- Originating web page
- http://divisionsbc.ca/provincial/resources/assessment-measurement/mapping-current-situation
- Description
- This article describes how to capture the patient experience and it is important
Central Okanagan Division of Family Practice – Engagement Journey
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource1569
- Division
- Central Okanagan Division of Family Practice
- Published Date
- 2017
- Description
- "This is the Central Okanagan Division of Family Practice’s PMH Engagement Journey. The PMH Engagement Journeys were designed to capture eight divisions' early implementation of the patient medical home (PMH) model of health care. The stories offer a look at the challenges and successes the divisions experienced along their journeys, and the resources they created to engage members and partners around primary care. It is the hope that these stories will act as a resource, support, and source of inspiration for other divisions beginning their journeys to an integrated system of care via the PMH."
- Division
- Central Okanagan Division of Family Practice
- Corporate Author
- Central Okanagan Division of Family Practice
- General Practice Services Committee
- Published Date
- 2017
- Topics
- Engagement
- Patient Medical Home
- Resource Type
- Case Study
- File Type
- Description
- This is the Central Okanagan Division of Family Practice’s PMH Engagement Journey. The PMH Engagement Journeys were designed to capture eight divisions' early implementation of the patient medical home (PMH) model of health care. The stories offer a look at the challenges and successes the divisions experienced along their journeys, and the resources they created to engage members and partners around primary care. It is the hope that these stories will act as a resource, support, and source of inspiration for other divisions beginning their journeys to an integrated system of care via the PMH.
Change Concepts and Ideas
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource1379
- Published Date
- 2016
- Link to File
- http://www.hqontario.ca/Portals/0/Documents/qi/qi-change-concepts-and-ideas-primer-en.pdf
- Description
- "This workbook goes into slightly more detail explaining some of the key change concepts"
- Corporate Author
- Health Quality Ontario
- Published Date
- 2016
- Topics
- Quality Improvement
- Resource Type
- Workbook
- File Type
- Link to File
- http://www.hqontario.ca/Portals/0/Documents/qi/qi-change-concepts-and-ideas-primer-en.pdf
- Originating web page
- http://divisionsbc.ca/provincial/resources/assessment-measurement/changes-concepts-ideas
- Description
- This workbook goes into slightly more detail explaining some of the key change concepts