5 public records – page 1 of 1. — Log in to view all records
Project Coordinator, A GP for Me Sunshiner's Frailty Network
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource429
- Health Authority
- Fraser
- Division
- Fraser Northwest Division of Family Practice
- Program
- A GP for Me
- Description
- "Job description for the Fraser Northwest Division's A GP for me Sunshiner's Frailty Network project coordinator."
- Health Authority
- Fraser
- Division
- Fraser Northwest Division of Family Practice
- Program
- A GP for Me
- Corporate Author
- Fraser Northwest Division of Family Practice
- Topics
- Patient Medical Home
- PMH Attributes: TBC Toolkit - Understanding TBC
- Frail Patients
- Human Resources
- Seniors
- Team-Based Care
- Nurse Practitioners
- Resource Type
- Job Description
- File Type
- Description
- Job description for the Fraser Northwest Division's A GP for me Sunshiner's Frailty Network project coordinator.
Cost Analysis of a Nurse Practitioner in a GP Clinic
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource509
- Health Authority
- Vancouver Coastal
- Division
- Powell River Division of Family Practice
- Program
- A GP for Me
- Published Date
- 2015-12-22
- Description
- "This document examines the financial impact of the work environment of a Nurse Practitioner (NP) on Vancouver Coastal Health’s (VCH) budget. It evaluates the cost effectiveness of having the NP work from a General Practitioners (GP) clinic compared to the community healthcare clinic in the hospital. NPs are working in many different primary care areas, as a specialist or as generalist in a primary care setting. Compared to physicians, patient satisfaction and quality of care have been equal or higher than care provided by physicians. NPs are effective in the reduction of patient unattachment and reduction of emergency department (ED) visits. Although NPs take often more consultation time and sometimes conduct more preventative actions, their work can be comparable or even more effective compared to other providers. This study hypothesized that the NP’s direct patient time and accessibility increases in the GP clinic, leading to a reduction of ED cost. ED and hospitalization cost of NP patients one year prior to attachment is compared with one year after attachment. Cost effectiveness is calculated by deducting incremental work environment cost by avoided ED and hospitalization cost."
- Health Authority
- Vancouver Coastal
- Division
- Powell River Division of Family Practice
- Program
- A GP for Me
- Corporate Author
- Powell River Division of Family Practice
- Personal Author
- Christien Kaaij
- Published Date
- 2015-12-22
- Resource Type
- Report
- File Type
- Description
- This document examines the financial impact of the work environment of a Nurse Practitioner (NP) on Vancouver Coastal Health’s (VCH) budget. It evaluates the cost effectiveness of having the NP work from a General Practitioners (GP) clinic compared to the community healthcare clinic in the hospital. NPs are working in many different primary care areas, as a specialist or as generalist in a primary care setting. Compared to physicians, patient satisfaction and quality of care have been equal or higher than care provided by physicians. NPs are effective in the reduction of patient unattachment and reduction of emergency department (ED) visits. Although NPs take often more consultation time and sometimes conduct more preventative actions, their work can be comparable or even more effective compared to other providers. This study hypothesized that the NP’s direct patient time and accessibility increases in the GP clinic, leading to a reduction of ED cost. ED and hospitalization cost of NP patients one year prior to attachment is compared with one year after attachment. Cost effectiveness is calculated by deducting incremental work environment cost by avoided ED and hospitalization cost.
Improving Ongoing Care for High-Risk Patients
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource510
- Health Authority
- Vancouver Coastal
- Division
- Powell River Division of Family Practice
- Program
- A GP for Me
- Published Date
- 2015-12-22
- Link to File
- /media/divresources/NPArticlePowellRiver.pdf
- Description
- "Article to raise awareness about Nurse Practitioner (NP) in Powell River. To support better care for patients, the Powell River Division and Vancouver Coastal Health piloted a new program to refer patients with chronic conditions to a nurse practitioner. Nurse practitioners can order and interpret diagnostic tests, make medical diagnoses, prescribe some medications, perform specific procedures, and refer to medical specialists."
- Health Authority
- Vancouver Coastal
- Division
- Powell River Division of Family Practice
- Program
- A GP for Me
- Corporate Author
- Powell River Division of Family Practice
- Personal Author
- Christien Kaaij
- Published Date
- 2015-12-22
- Resource Type
- Article
- File Type
- Link to File
- /media/divresources/NPArticlePowellRiver.pdf
- Description
- Article to raise awareness about Nurse Practitioner (NP) in Powell River. To support better care for patients, the Powell River Division and Vancouver Coastal Health piloted a new program to refer patients with chronic conditions to a nurse practitioner. Nurse practitioners can order and interpret diagnostic tests, make medical diagnoses, prescribe some medications, perform specific procedures, and refer to medical specialists.
BC PMH Practice Characteristics Matrix with Cover Page
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource1081
- Program
- Practice Support Program
- Published Date
- 04-20-2018
- Description
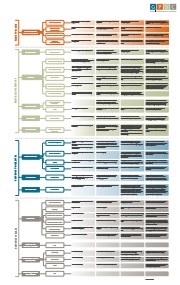
- "The PMH Practice Characteristics Matrix supports physicians to understand what the 12 attributes of the PMH model mean in concrete terms in the context of their practice, and what a transition towards the PMH could entail for them. As well, it helps GPSC and other health system partners to organize their thinking around the practice-level realities of the PMH model, and the strategic development of provincial supports for physicians to achieve the model. The Matrix—intended to be read from left to right--illustrates both the 12 attributes of the PMH model, as well as their corresponding sub-attributes, several of which are to be achieved cumulatively."
- Program
- Practice Support Program
- Corporate Author
- General Practice Services Committee
- Published Date
- 04-20-2018
- Topics
- Patient Medical Home
- Resource Type
- Report
- File Type
- Description
- The PMH Practice Characteristics Matrix supports physicians to understand what the 12 attributes of the PMH model mean in concrete terms in the context of their practice, and what a transition towards the PMH could entail for them. As well, it helps GPSC and other health system partners to organize their thinking around the practice-level realities of the PMH model, and the strategic development of provincial supports for physicians to achieve the model. The Matrix—intended to be read from left to right--illustrates both the 12 attributes of the PMH model, as well as their corresponding sub-attributes, several of which are to be achieved cumulatively.
BC PMH Practice Characteristics Matrix Poster
https://www.jcc-resourcecatalogue.ca/en/permalink/divisionresource1082
- Program
- Practice Support Program
- Published Date
- 2018-04-20
- Description
- "The PMH Practice Characteristics Matrix supports physicians to understand what the 12 attributes of the PMH model mean in concrete terms in the context of their practice, and what a transition towards the PMH could entail for them. As well, it helps GPSC and other health system partners to organize their thinking around the practice-level realities of the PMH model, and the strategic development of provincial supports for physicians to achieve the model. The Matrix—intended to be read from left to right--illustrates both the 12 attributes of the PMH model, as well as their corresponding sub-attributes, several of which are to be achieved cumulatively."
- Program
- Practice Support Program
- Corporate Author
- General Practice Services Committee
- Published Date
- 2018-04-20
- Topics
- Patient Medical Home
- Resource Type
- Poster
- File Type
- Description
- The PMH Practice Characteristics Matrix supports physicians to understand what the 12 attributes of the PMH model mean in concrete terms in the context of their practice, and what a transition towards the PMH could entail for them. As well, it helps GPSC and other health system partners to organize their thinking around the practice-level realities of the PMH model, and the strategic development of provincial supports for physicians to achieve the model. The Matrix—intended to be read from left to right--illustrates both the 12 attributes of the PMH model, as well as their corresponding sub-attributes, several of which are to be achieved cumulatively.